If you have diabetes and are considering dental implants, the question is usually not just can it be done, but can it be done safely. The short answer is yes. The more important answer depends on how well the condition is managed and how the treatment is planned.
This guide explains what people with diabetes should know before getting dental implants, how safety and success are evaluated, and what factors make the biggest difference in long-term results.
At Elizabeth L. Wakim DDS, we take a personalized approach to implant planning for patients with diabetes. Our comprehensive consultations consider overall health, oral conditions, and imaging findings to create treatment plans that support safe healing and long-term stability.
How Dental Implants Work
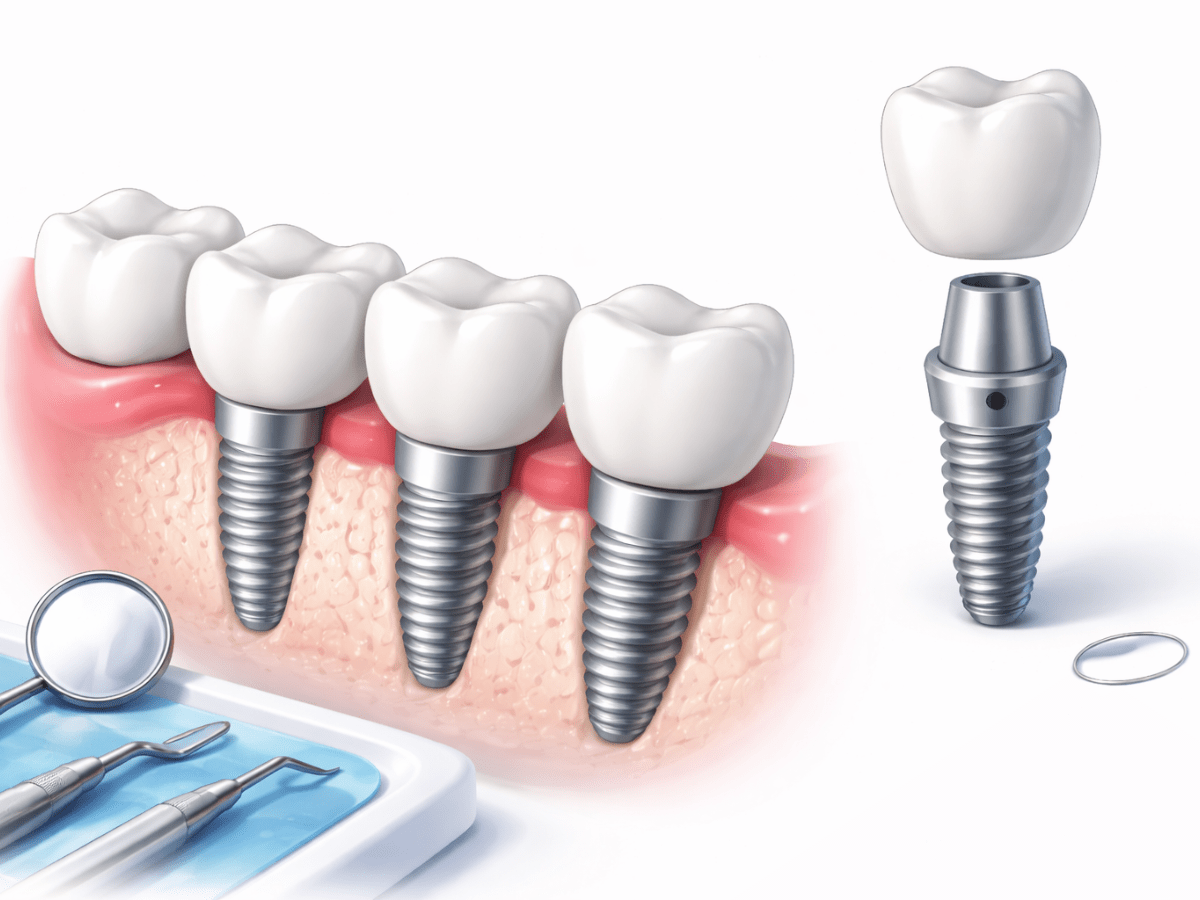
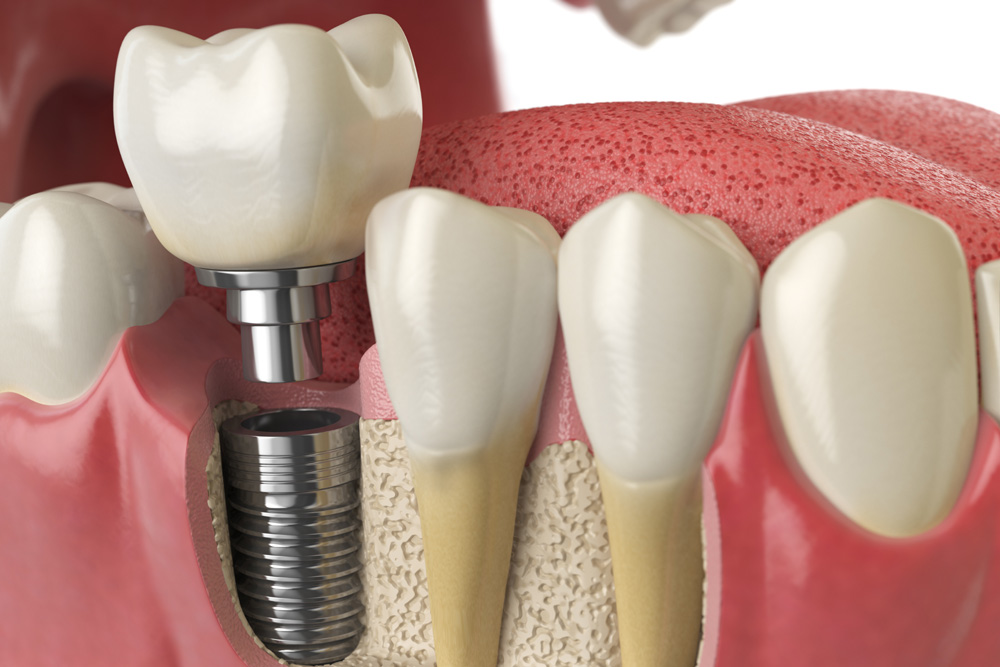
Dental implants replace missing teeth by mimicking the structure of a natural tooth. The implant itself is a small titanium post placed into the jawbone that acts as an artificial root. This post is called the fixture. Once the fixture is placed, it needs time to fuse with the surrounding bone in a process called osseointegration.
After the implant has integrated with the bone, a connector piece known as the abutment is attached. The abutment supports the final component, the crown, which is custom-made to look and function like a natural tooth.
Why Diabetes Matters for Dental Implants
Diabetes can influence dental implant success because it affects several processes the body relies on for healing and infection control.
- Slower wound healing: Elevated blood sugar levels can delay the body’s ability to repair tissue after surgery, which may extend healing time around the implant site.
- Reduced immune response: Diabetes can weaken the immune system’s response to bacteria, increasing the risk of infection in the gums and surrounding bone during recovery.
- Differences between well-controlled and poorly controlled diabetes: People with well-controlled diabetes often heal similarly to individuals without diabetes. Poorly controlled diabetes is linked to higher infection risk, slower healing, and increased implant complications.
- Blood sugar control and surgical outcomes: Stable blood sugar levels support healthy bone remodeling and tissue repair, which are essential for the implant to properly fuse with the jawbone and remain stable long term.
Because of these factors, careful medical evaluation and blood sugar management play an important role in determining whether dental implants are a safe and effective option for patients with diabetes. This type of personalized assessment is a key part of comprehensive dental implant care, helping ensure treatment decisions support proper healing, long-term stability, and overall oral health.
Types of Diabetes and Implant Considerations
With more than 589 million people worldwide living with diabetes, it is important to recognize that not all forms of diabetes affect dental implant treatment in the same way. Understanding the type of diabetes and how well it is managed helps guide safe planning and long-term implant success.
Type 1 Diabetes
Type 1 diabetes is an autoimmune condition that requires lifelong insulin management. Dental implants may be an option when blood sugar levels are well controlled, but careful evaluation and coordination with a patient’s medical provider are often recommended to support healing and reduce infection risk.
Type 2 Diabetes
Type 2 diabetes is the most common form and can vary widely in severity. Patients with well-managed Type 2 diabetes often experience implant outcomes similar to those without diabetes. Poor blood sugar control, however, can increase the risk of delayed healing and post-surgical complications.
Prediabetes
Prediabetes involves elevated blood sugar levels that are not yet in the diabetic range. Many individuals with prediabetes are good candidates for dental implants, particularly when preventive care and healthy lifestyle habits are in place to support healing.
Rather than focusing on the diagnosis alone, dentists assess overall blood sugar control, oral health, and bone quality to determine whether dental implants can be placed safely and successfully.
How to Manage Blood Sugar for Dental Implant Surgery
Many dentists prefer patients to have an A1C below 7 percent before proceeding with dental implants. This level is associated with better surgical outcomes and lower complication risk. In some cases, slightly higher levels may still be considered if diabetes is stable and closely managed.
Practical Ways to Manage Glucose Before and After Surgery
Patients can take several steps to support safe healing and implant success.
- Monitor blood sugar consistently before surgery: Tracking glucose levels in the weeks leading up to treatment helps identify patterns that may affect healing. Your oral surgeon may also review recent blood test results as part of your medical history and health history.
- Follow medication or insulin plans exactly as prescribed: Stable glucose levels support proper healing after implant placement. Uncontrolled diabetes increases the risk of bone loss, gum health complications, and delayed healing compared to non diabetic individuals.
- Maintain a balanced diet that supports steady glucose levels: Nutrient-rich foods help protect bone density and reduce inflammation, which is important when artificial tooth roots are integrating with the jawbone.
- Practice excellent oral hygiene every day: Keeping the mouth clean helps prevent infection, reduces plaque buildup, and protects gum tissue during recovery. Strong oral health diabetes habits lower the risk of complications around the implant site.
- Attend all follow-up visits and follow post operative care instructions: Follow-up care allows your dental team to monitor bone health, gum healing, and early signs of concern. This is especially important for patients with a history of tooth loss, kidney disease, vision loss, or other conditions that may affect healing.
Effective blood sugar management helps improve healing, reduce complications, and support long-term implant stability. These outcomes are closely tied to ongoing preventive dentistry practices that focus on early intervention, routine monitoring, and maintaining overall oral health throughout treatment and recovery.
Healing Timeline and What’s Normal
Healing after dental implant surgery happens in stages. Understanding what is normal can help patients feel more confident during recovery and know when to check in with their dental provider.
Soft Tissue Healing
In the first few days after surgery, mild swelling, tenderness, and slight bleeding are common. The gums typically begin to seal around the implant site within the first one to two weeks. During this time, discomfort should gradually decrease, and the area should start to feel more stable.
Bone Integration
Dental implants begin integrating with the jawbone soon after placement through a process called osseointegration. This phase usually takes several months. As bone grows around the implant, it becomes firmly anchored, creating the foundation needed to support the final restoration.
When to See a Dentist During Implant Healing
For many patients, the dental implant process follows a steady and predictable healing process. However, certain symptoms may signal an increased risk of implant failure and should be evaluated promptly.
Contact your dentist if you notice any of the following:
- Increasing pain or swelling after the first few days, which may indicate delayed healing or infection
- Persistent bleeding or discharge around the implant site that does not improve
- Redness or warmth affecting the surrounding gums, which can be an early sign of gum disease or inflammation
- A feeling that the titanium implant is loose or shifting, which may affect bone structure and implant stability
- Fever or signs of infection, particularly in patients with high blood sugar levels or reduced body’s healing ability
Reaching out to your dental provider early allows potential concerns to be addressed before they impact long-term results. With proper monitoring, many patients are able to receive dental implants safely and enjoy a permanent solution that supports dental health, unlike dentures or dental bridges.
Making an Informed Decision About Dental Implants With Diabetes
Diabetes does not automatically prevent someone from getting dental implants. What matters most is how well the condition is managed and how carefully treatment is planned. When blood sugar is controlled, oral health is stable, and healing capacity is properly evaluated, dental implants can be a safe and reliable option for replacing missing teeth.
Successful outcomes depend on personalized planning, realistic expectations, and consistent aftercare. Monitoring blood sugar, maintaining good oral hygiene, and attending follow-up visits all play an important role in long-term implant stability, which is a core focus of comprehensive restorative dentistry aimed at preserving function, comfort, and oral health over time.
Our team is committed to providing safe, personalized dental implant care for patients with diabetes. If you have questions about implant eligibility, healing, or how blood sugar management may affect your treatment, we are here to help. Contact our Pennsylvania office at (724) 558-8222 or use our contact form to schedule a consultation and receive guidance tailored to your oral health and overall wellness needs.

Dr. Elizabeth Wakim, DDS, is the founder of Enhanced Wellness. She’s a compassionate and highly-regarded dentist with her own practice in Washington, Pennsylvania, known for providing modern, comprehensive dental care, botox and facial aesthetics with a focus on patient comfort and anxiety reduction, serving general, cosmetic, and pediatric dentistry needs.