Jaw clicking when you chew. Tension along your temples. A headache that won’t fully go away. Then out of nowhere, a brief spinning sensation. When jaw symptoms and dizziness show up together, the connection feels hard to ignore. Does TMJ cause vertigo?
Before assuming anything, though, it helps to understand how balance actually works and where TMJ fits into that system. Let’s look at what the evidence actually shows and how to decide if your jaw could be part of the equation.
At Elizabeth L. Wakim DDS, TMJ evaluations go beyond checking for jaw pain. A thorough assessment looks at bite alignment, muscle tension, joint function, and how those factors may interact with surrounding structures. The goal is clarity. If the jaw is involved, we address it. If something else is driving the symptoms, that matters just as much.
What Is TMJ (Temporomandibular Joint Disorder)?
The temporomandibular joint, or TMJ, is the hinge that connects your lower jawbone to your skull. You have one on each side of your head, positioned just in front of your ears. These joints allow you to chew, speak, yawn, and move your jaw smoothly in multiple directions.
When this system becomes irritated or dysfunctional, it’s referred to as temporomandibular joint disorder, or TMD. It’s more common than many people realize. Research estimates that TMD affects roughly 5% to 12% of the population, which translates to approximately 33 million Americans.
Most people who say, “I have TMJ,” are actually referring to TMD, short for temporomandibular disorder. TMJ is the name of the joint itself. TMD describes dysfunction involving the joint, surrounding muscles, or bite alignment. That distinction matters because symptoms do not always originate from the joint alone. Muscle tension, inflammation, or alignment issues within the system can all contribute to discomfort.
TMD is more than simple jaw pain. It can involve:
- Jaw soreness or tenderness
- Clicking, popping, or grinding sounds
- Limited jaw movement or locking
- Facial tension or temple headaches
- Ear-related symptoms such as fullness or pressure
Because the joint sits close to the ear and shares muscle and nerve pathways with nearby structures, symptoms can sometimes extend beyond the jaw. Understanding how TMJ disorders are associated with orofacial pain helps clarify why discomfort may radiate to the temples, ears, or face. That broader perspective explains why TMJ conditions are evaluated carefully, especially when symptoms don’t seem limited to the mouth.
Vertigo vs. Dizziness: What’s the Difference?
People often use “vertigo” and “dizziness” interchangeably, but they are not the same thing.
Dizziness is a broad term. It can describe feeling lightheaded, faint, unsteady, foggy, or off-balance. It may be related to blood pressure changes, dehydration, anxiety, medication side effects, or inner ear issues.
Vertigo, on the other hand, is specific. It’s the sensation that you or your surroundings are spinning or moving when they’re not. Some people describe it as the room tilting, shifting, or rotating. Each year, vertigo affects an estimated 15% to 20% of adults, making it a relatively common balance complaint. It is most often linked to problems in the inner ear or the brain’s balance centers.
Being precise about what you’re feeling helps narrow down possible causes and avoids chasing the wrong explanation.
Can TMJ Cause Vertigo? What We Know and How It Might Happen
The temporomandibular joint sits just in front of the ear, near the structures responsible for balance. Studies show that dizziness and vertigo are reported more often in people with temporomandibular disorders than in the general population. Some research estimates that 30% to 60% of individuals with TMD report balance-related symptoms.
That said, this reflects an association, not automatic causation. Inner ear conditions remain the most common cause of true vertigo. When TMJ is involved, it is usually one piece of a larger puzzle.
So how could the jaw influence balance?
Inner Ear Signaling Interference
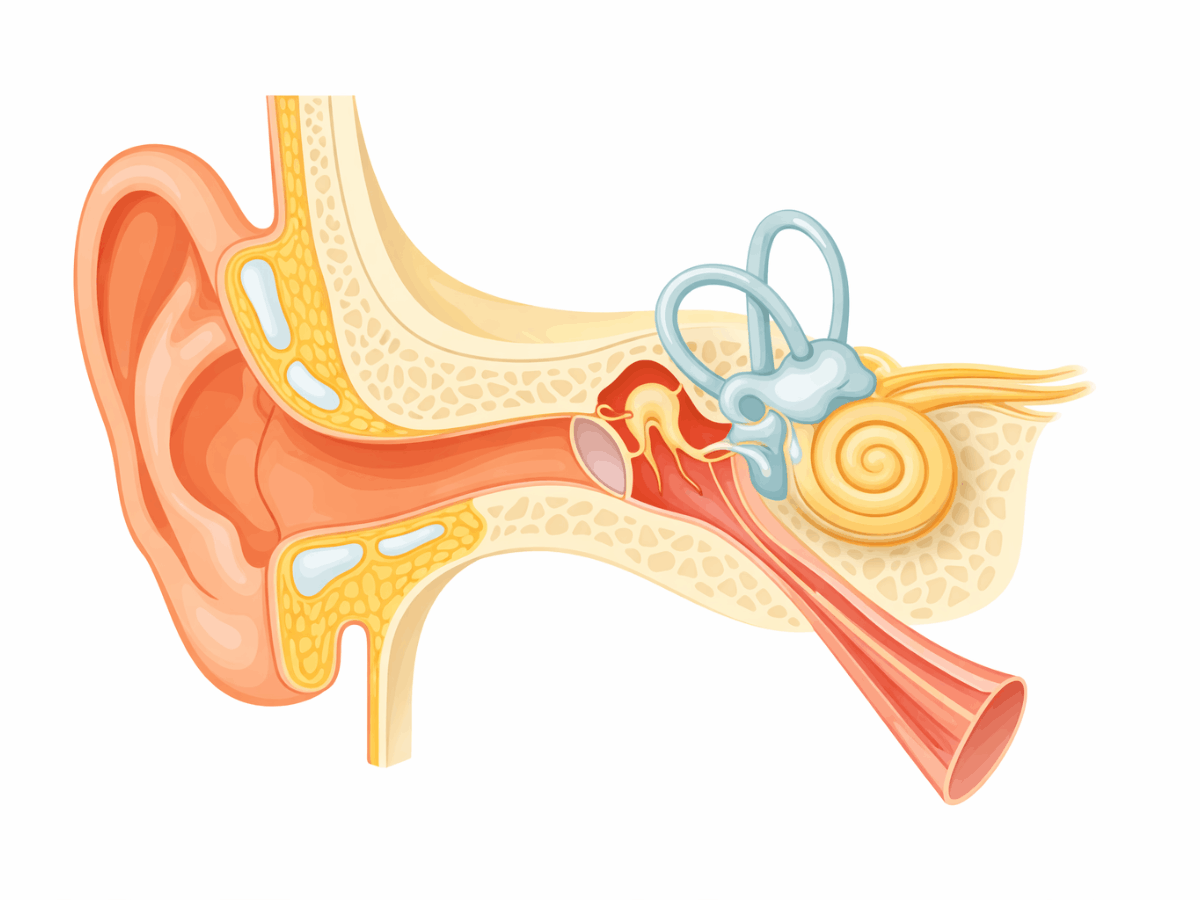
The jaw joint and nearby muscles share nerve pathways with structures close to the vestibular system. Chronic inflammation or altered jaw mechanics may affect how sensory signals are processed.
For some people, this may feel like brief spinning episodes or subtle instability, especially during jaw movement.
Muscle Tension and the Neck-Jaw Connection
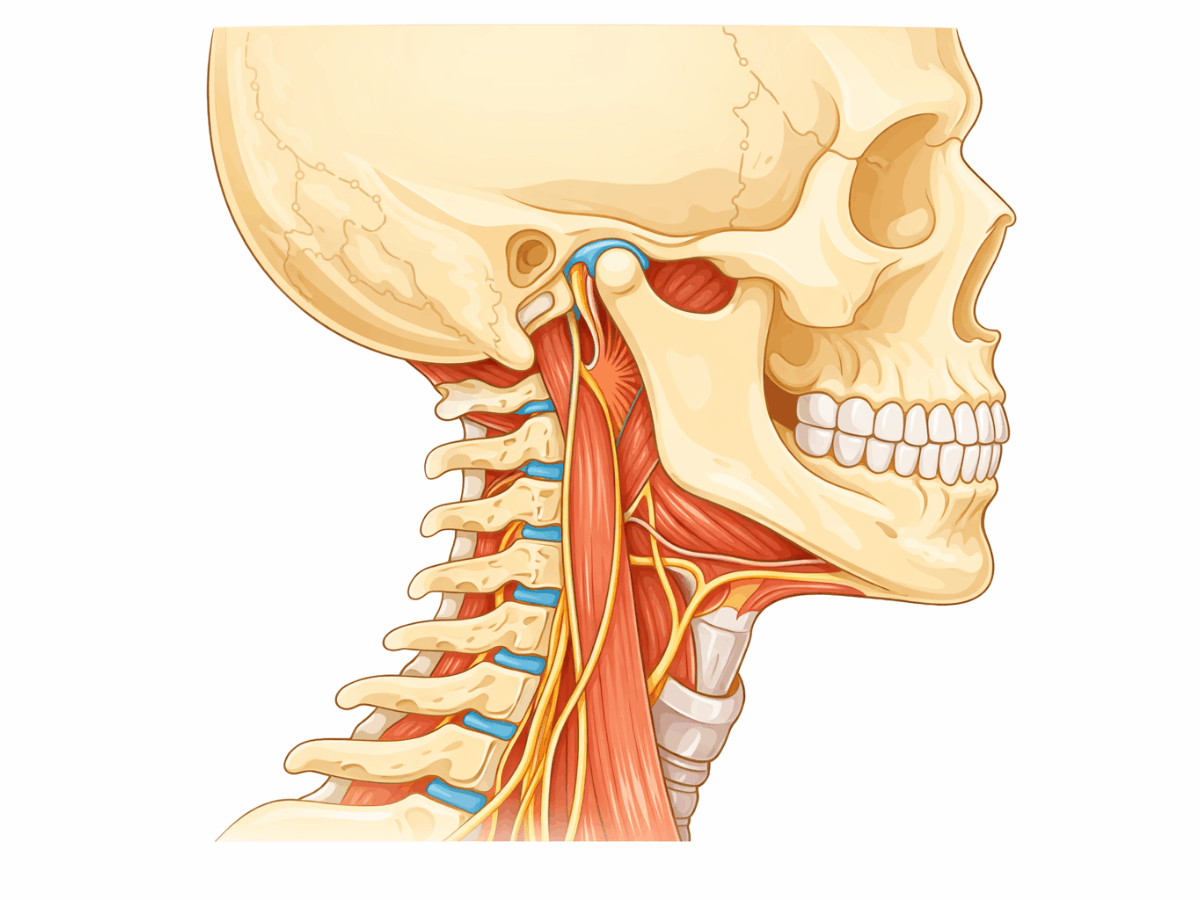
The muscles that control the jaw are closely connected to the neck and upper cervical spine. Those areas play a role in spatial awareness and balance.
If you notice dizziness during prolonged clenching, stress, or after chewing for long periods, muscular strain could be contributing.
Pressure Around Ear Structures
Inflammation in the TMJ area can create a sensation of fullness or pressure near the ear. While this does not directly damage the inner ear, it may influence nearby tissues and sensory perception in certain individuals.
Jaw Alignment and Posture
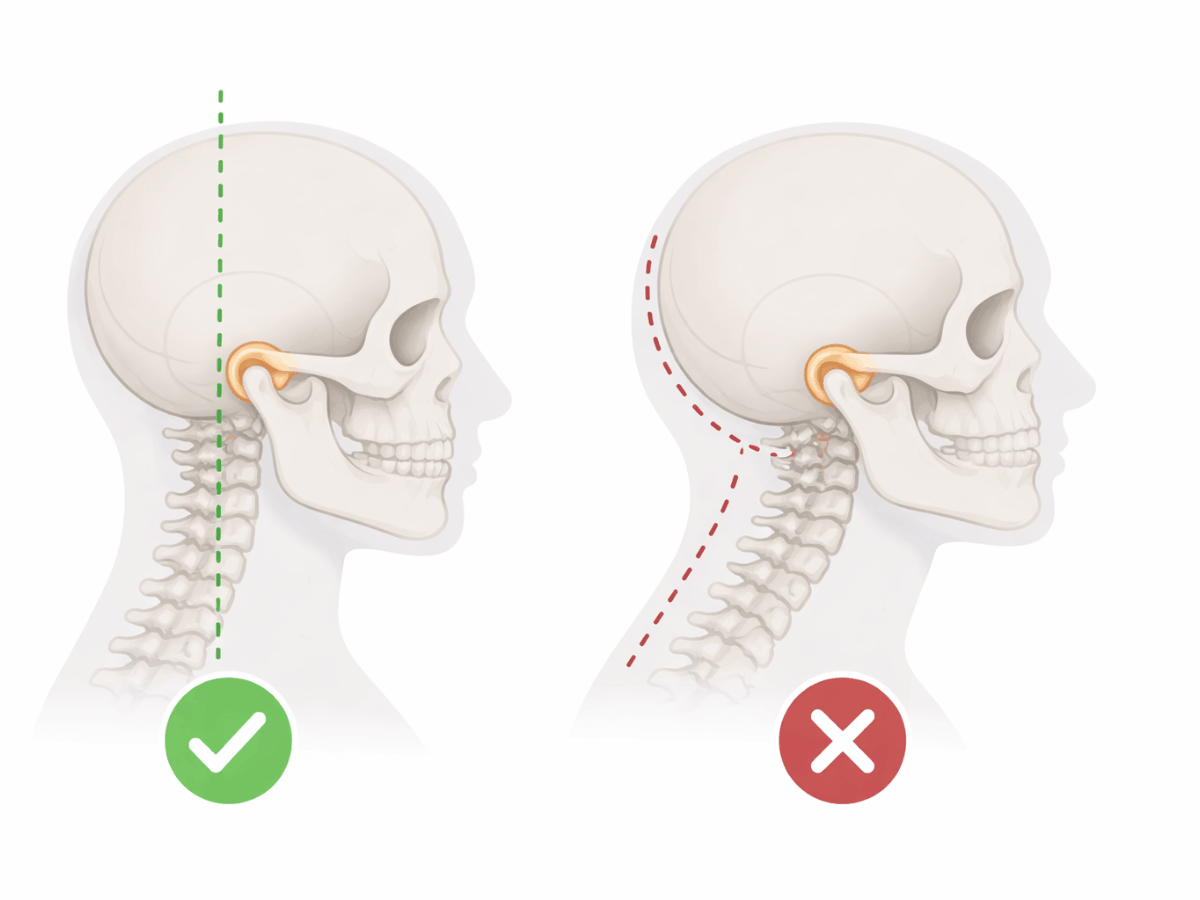
Your bite affects head and neck positioning. Subtle alignment issues can influence muscle recruitment patterns in the upper body. Over time, that altered input may affect how your brain integrates balance signals.
This doesn’t mean every bite issue causes vertigo. In some cases, muscle-relaxing treatments such as Botox for TMJ are used to reduce excessive jaw tension. But structural imbalance or chronic muscle strain may contribute to instability in certain individuals.
Symptoms That Might Suggest a TMJ-Related Vertigo Link
Some patterns may point toward TMJ dysfunction contributing to balance issues:
Spinning sensation when moving your head or jaw: The room feels like it shifts briefly when you turn your head, yawn, or open wide. This type of vertigo caused by movement may overlap with certain TMJ symptoms.
Balance changes without a clear trigger: You feel slightly unsteady or off balance, even though you are not sick or dehydrated. Subtle balance problems like this can sometimes occur alongside chronic TMJ issues.
Dizziness during chewing or clenching: Symptoms appear after long meals, gum chewing, or periods of jaw tension. Ongoing teeth grinding or muscle strain may increase pressure around the joint.
Ear fullness, ringing, or pressure: A clogged or tight sensation near the ear that comes and goes with TMJ pain or jaw tenderness. These ear symptoms are common in some TMJ sufferers.
Neck tightness paired with dizziness: Stiffness at the base of the skull or along the sides of the neck when you feel dizzy. Poor posture and jaw tension can affect how the body regulates balance and spatial awareness.
These symptoms do not confirm the root cause, but when they occur together, they may suggest that TMJ-related dizziness deserves closer evaluation.
Other Conditions That Can Cause Vertigo (and Why to Rule Them Out)
TMJ can contribute to certain symptoms, but it is not the most common cause of vertigo. Several inner ear and neurological conditions are more directly linked to balance disruption. Before assuming the jaw is responsible, these possibilities should be considered.
Ménière’s Disease
Ménière’s disease affects the inner ear and can cause recurring vertigo episodes, hearing changes, ringing in the ear, and a feeling of fullness. Because TMJ can also create ear pressure and tinnitus, the overlap in symptoms sometimes leads to confusion. The difference is that Ménière’s disease originates within the inner ear itself.
Benign Paroxysmal Positional Vertigo (BPPV)
BPPV is one of the most common causes of vertigo. It occurs when small calcium crystals in the inner ear shift out of position. Episodes are usually brief and triggered by head movement, such as rolling over in bed or looking up. Since some people with TMJ notice dizziness during jaw or head movement, BPPV is sometimes mistaken for a jaw-related issue.
Vestibular Migraines
Vestibular migraines are a recognized cause of episodic vertigo and are estimated to affect about1% to 3% of the general population. Unlike classic migraines, they may not always involve severe head pain. Instead, symptoms can include spinning sensations, motion sensitivity, imbalance, light sensitivity, or nausea.
Inner Ear Infections or Inflammation
Conditions such as labyrinthitis or vestibular neuritis can cause sudden, intense vertigo, often accompanied by nausea or imbalance. These conditions involve inflammation of the vestibular system. If vertigo appears abruptly and is severe, an inner ear condition is more likely than TMJ.
True vertigo most often originates from the vestibular system. TMJ may contribute in certain cases, but a careful evaluation helps ensure the correct system is being treated.
Treatment Approaches That Help Both TMJ and Vertigo Symptoms
If TMJ is contributing to balance-related symptoms, treatment focuses on reducing joint strain, calming muscle tension, and restoring proper jaw function. The goal is not just pain relief, but improved neuromuscular stability.
Lifestyle Adjustments and Jaw Habits
Small daily habits can significantly reduce joint stress. This may include:
- Avoiding gum chewing and hard or chewy foods
- Limiting wide mouth opening during yawning
- Becoming aware of daytime clenching or teeth contact
- Using gentle heat to relax tight jaw muscles
Reducing repetitive strain can lower inflammation and muscle overactivity, which may decrease associated dizziness in some patients.
Physical Therapy and Targeted Jaw Exercises
Physical therapy for TMD often includes guided stretching, strengthening, and coordination exercises for the jaw and neck. Therapists may also address upper cervical spine mobility, since neck dysfunction can influence balance perception.
Manual therapy techniques can reduce muscle tension in the masseter, temporalis, and surrounding cervical muscles. For patients whose dizziness is linked to muscular strain, improving joint mechanics can reduce symptom frequency.
Oral Appliances or Night Guards
Custom oral appliances are designed to stabilize the bite and reduce nighttime clenching or grinding. By decreasing excessive pressure on the joint and surrounding muscles, appliances may reduce inflammation and neuromuscular irritation.
It’s important that these devices are professionally fitted. Over-the-counter guards may not address alignment properly and can sometimes worsen symptoms.
Posture and Neck Support
Forward head posture and prolonged screen use increase strain on both the jaw and upper cervical spine. Supporting proper head and neck alignment during work and sleep can reduce muscle tension that contributes to both TMJ discomfort and balance complaints.
Simple changes such as ergonomic adjustments, cervical support pillows, and posture awareness can improve muscular coordination over time.
When Medical Evaluation Is Necessary
If vertigo is persistent, severe, associated with hearing loss, neurological symptoms, or sudden onset imbalance, a medical evaluation should come first. An ENT or neurologist may need to rule out vestibular disorders before TMJ treatment is pursued.
In some cases, minimally invasive options such as Botox TMJ treatment for jaw pain may be considered when muscle tension is a contributing factor. When TMJ and vestibular factors overlap, collaborative care may provide the best outcome.
When Symptoms Overlap, Precision Matters
Jaw discomfort and vertigo can appear together, but proximity alone does not confirm causation. The temporomandibular joint sits near structures involved in balance, and in some individuals, muscle tension, inflammation, or bite instability may contribute to balance-related symptoms. That possibility deserves thoughtful evaluation, not assumptions.
At Elizabeth L. Wakim DDS, our approach to TMD treatment begins with a comprehensive, individualized assessment. TMJ evaluations look closely at joint mechanics, muscle function, and bite alignment while also considering the broader clinical picture. If you’re experiencing persistent jaw discomfort, facial tension, or balance-related symptoms, scheduling an evaluation can help determine the appropriate course of care. Contact our Pennsylvania office at (724) 558-8222 or use our contact form to request a consultation.

Dr. Elizabeth Wakim, DDS, is the founder of Enhanced Wellness. She’s a compassionate and highly-regarded dentist with her own practice in Washington, Pennsylvania, known for providing modern, comprehensive dental care, botox and facial aesthetics with a focus on patient comfort and anxiety reduction, serving general, cosmetic, and pediatric dentistry needs.