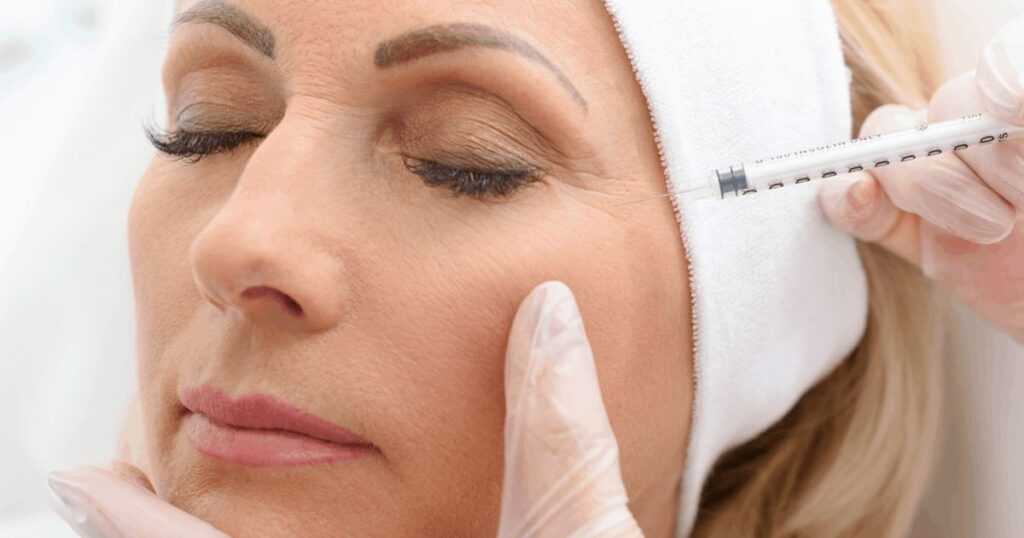
Jaw tension, morning headaches, and that dull ache that follows hours of clenching can make daily life uncomfortable. TMJ discomfort often affects how you chew, speak, and even rest, sometimes without realizing how much strain your jaw is under.
More patients are exploring a treatment that’s gaining attention in both dental and wellness circles. Jaw Botox for TMJ is being used to relax overworked jaw muscles, relieve pressure, and ease pain. But how effective is it, and what can patients realistically expect from treatment?
At Elizabeth L. Wakim DDS, we use evidence-based techniques to help patients find lasting relief from TMJ pain. Our approach combines modern diagnostic tools with personalized care to ensure every treatment plan supports both comfort and long-term oral health.
Understanding TMJ and Why the Jaw Locks Up

The temporomandibular joint, or TMJ, works like a hinge that connects your jawbone to your skull. It allows you to speak, chew, and yawn. When this joint or the surrounding muscles become strained or inflamed, it can lead to temporomandibular joint disorder, often called TMJ.
Common symptoms include jaw stiffness, popping or clicking sounds, headaches, ear pressure, and soreness in the cheeks or temples. These following symptoms often appear gradually and can worsen during stressful periods or after long hours of clenching or grinding your teeth. Further explanation is provided in this article on TMJ vs. TMD which clarifies how such symptoms relate to the joint versus the disorder.
Common Causes of TMJ Pain
TMJ discomfort can develop from several contributing factors. Identifying what triggers your symptoms helps determine the most effective treatment plan.
- Chronic teeth grinding or clenching that overworks the jaw muscles and leads to chronic facial pain, myofascial pain, and tension-related neck pain.
- A misaligned bite or dental issues that place uneven pressure on the joint and surrounding muscles.
- Stress and muscle tension that trigger unconscious jaw tightening or repeated muscle spasms during the day or while sleeping.
- Arthritis or inflammatory conditions that affect how smoothly the temporomandibular joint (TMJ) moves.
- Previous jaw injury or trauma that disrupts normal function and may require more advanced TMJ treatment or even other treatments like oral appliances.
- Connective tissue disorders or medical conditions that weaken joint stability and make it harder for the jaw to move without pain.
When managed properly, most patients achieve significant relief without the need for surgery, finding complete relief through personalized care that focuses on managing pain and restoring natural jaw function. This aligns with information on TMJ disorders associated with orofacial pain, which highlights the connection between joint dysfunction and muscle-related discomfort.
What Is Jaw Botox for TMJ and How It Works
An estimated 5 to 12 percent of people experience symptoms of temporomandibular joint (TMJ) disorders, often marked by jaw pain, clenching, and tension. Jaw Botox for TMJ targets the overactive muscles responsible for these symptoms. The treatment uses small, precise doses of botulinum toxin (Botox) to help the muscles relax, easing pressure on the joint and reducing discomfort over time.
When these muscles are chronically tight, they can cause headaches, jaw pain, and even tooth damage from grinding. By relaxing them, Botox helps reduce muscle strain and allows the temporomandibular joint to move more freely. The result is less pain, less tension, and a noticeable reduction in clenching.
How It Works
Studies show that Botox can be highly effective for temporomandibular joint (TMJ) disorders, with pain reduction rates between 50 and 90 percent in some patients. Botox helps manage TMJ symptoms by interrupting the cycle of tension and pain in the jaw muscles. When injected into specific areas, it limits muscle contractions and allows the jaw to rest naturally.
1. Targets Overworked Muscles
Botox injections are placed into the masseter and temporalis muscles, which control chewing and clenching. These muscles often become overworked in people treating TMJ symptoms or jaw tension. When used in small doses, approved Botox helps these muscles relax, easing tightness and reducing inflammation, similar to how other noninvasive approaches for TMD treatment help restore comfort and function in the jaw.
2. Reduces Pressure on the Joint
By calming muscle activity, Botox injections reduce the pressure placed on the temporomandibular joint (TMJ). This helps ease jaw stiffness, chronic migraines, and facial tension that often develop from clenching or grinding.
3. Prevents Further Strain
When the jaw muscles are relaxed, they can move more naturally and with less effort. This prevents further strain on the temporomandibular joint (TMJ) and surrounding tissues. Over time, the muscles adapt to a healthier pattern, which helps reduce myofascial pain, muscle fatigue, and other symptoms linked to treating TMJ disorders.
4. Offers Gradual, Noticeable Relief
Relief from TMJ treatment Botox develops gradually as the jaw muscles relax and inflammation subsides. Most patients begin to feel pain ease within a few days, with noticeable improvement over the following weeks.
While Botox is commonly associated with cosmetic treatments, it has proven to be an effective therapeutic option for managing TMJ pain caused by muscle overuse. When performed by a qualified dentist, it can provide safe, long-lasting relief and improve daily comfort.
When Jaw Botox for TMJ May Not Be the Right Choice
Jaw Botox for TMJ can help many patients find relief from muscle-related jaw pain, but it is not the best solution for everyone. The treatment works by relaxing overactive muscles, so it may not be effective for TMJ pain caused by joint damage or structural issues.
You may want to explore other options if you:
- Have joint-related TMJ problems, such as arthritis, disc displacement, or bone degeneration. Botox targets muscle tension, not the joint itself.
- Are pregnant or breastfeeding, since Botox is not recommended during these stages.
- Have a neuromuscular disorder, such as myasthenia gravis or ALS, which can increase the risk of unwanted side effects.
- Take certain medications, like muscle relaxants or blood thinners, without prior medical clearance.
- Have experienced allergic reactions or adverse effects from previous Botox treatments.
A dentist experienced in TMJ and facial muscle anatomy can determine whether your symptoms are muscle-based or joint-related. If Botox is not suitable, they can recommend alternative treatments such as oral appliances, physical therapy, or oral and maxillofacial surgery when structural correction is needed to restore jaw alignment and comfort.
What to Expect During a Jaw Botox for TMJ Appointment
Jaw Botox for TMJ is a quick, in-office procedure designed to ease muscle tension and relieve pain with minimal downtime. The process typically takes 10 to 30 minutes, depending on how many areas need treatment.
Before the Appointment
Your dentist will review your medical history, assess your TMJ symptoms, and examine your jaw muscles to determine the correct injection points. You may be advised to avoid alcohol, blood thinners, and anti-inflammatory medications for a few days beforehand to reduce bruising risk.
During the Treatment
Botox is injected into specific jaw muscles, most often the masseter, temporalis, or sometimes the pterygoid. The injections feel like small pinches and don’t require anesthesia, although a topical numbing gel may be used for comfort. The entire session is completed in one visit, and you can return to your regular activities immediately afterward.
After the Procedure
Mild tenderness, redness, or swelling at the injection sites can occur but typically fade within a day or two. To help the Botox settle properly, avoid rubbing your face, lying flat, or engaging in strenuous exercise for several hours after treatment. Most patients start noticing improvement within a few days, with the full effects appearing after two weeks.
Every injection plan is tailored to your specific muscle structure, ensuring safety, comfort, and natural movement while reducing TMJ-related pain.
How Jaw Botox for TMJ Works Over Time
Jaw Botox for TMJ is a minimally invasive procedure that offers gradual, steady pain relief rather than instant results. Most patients suffering from temporomandibular joint syndrome begin to feel relief within a few days as the treated muscles relax and tension eases.
Here’s what to expect after treatment:
- Initial relief: Mild improvement in jaw tightness or clenching may appear within a few days.
- Full effect: The best results are typically felt around two weeks after treatment when muscle activity is most balanced.
- Easier movement: Many patients find it easier to chew, speak, and relax the jaw without tension or stiffness.
- Secondary benefits: A softer, more relaxed jawline can appear as overworked muscles begin to rest.
- Duration of results: Relief usually lasts three to four months before muscle activity gradually returns. Regular maintenance can help results last longer.
- Complementary care: Pairing Botox with preventive strategies such as stress management, a custom night guard, or bite adjustments helps protect results and promote lasting comfort.
Each treatment plan focuses on safe, effective muscle relief that aligns with your overall dental health. The goal is to reduce discomfort while maintaining natural movement and balance.
Finding Lasting Relief from TMJ Pain
Jaw Botox for TMJ can be a helpful solution for patients struggling with chronic jaw tension, headaches, or clenching when other options have not worked. While it does not cure TMJ disorders, it can significantly reduce muscle strain and improve overall comfort when used as part of a comprehensive care plan that may include restorative dentistry to correct bite alignment and support long-term jaw stability.
At Elizabeth L. Wakim DDS, every treatment begins with understanding the root cause of your discomfort. We focus on gentle, effective care that protects your muscles, joints, and overall oral health. If you’re dealing with persistent TMJ pain or tension, call our Pennsylvania office at (724) 558-8222 or use our contact form to schedule a consultation and explore personalized options for lasting relief.

Dr. Elizabeth Wakim, DDS, is the founder of Enhanced Wellness. She’s a compassionate and highly-regarded dentist with her own practice in Washington, Pennsylvania, known for providing modern, comprehensive dental care, botox and facial aesthetics with a focus on patient comfort and anxiety reduction, serving general, cosmetic, and pediatric dentistry needs.